I wrote before about how emergency medicine is, in my opinion, a dying field. Maybe it’s already dead. Emergency departments and their physicians have lost the war on multiple fronts: declining reimbursement from payers, declining interest from medical students, pay cuts, increasing liability, encroachment from midlevel providers, and a lack of offramps. To spare your attention span, here are some bullet points – facts, not opinions.
Continue readingFollowing the Money…?
I have a really good job for an ER doctor.
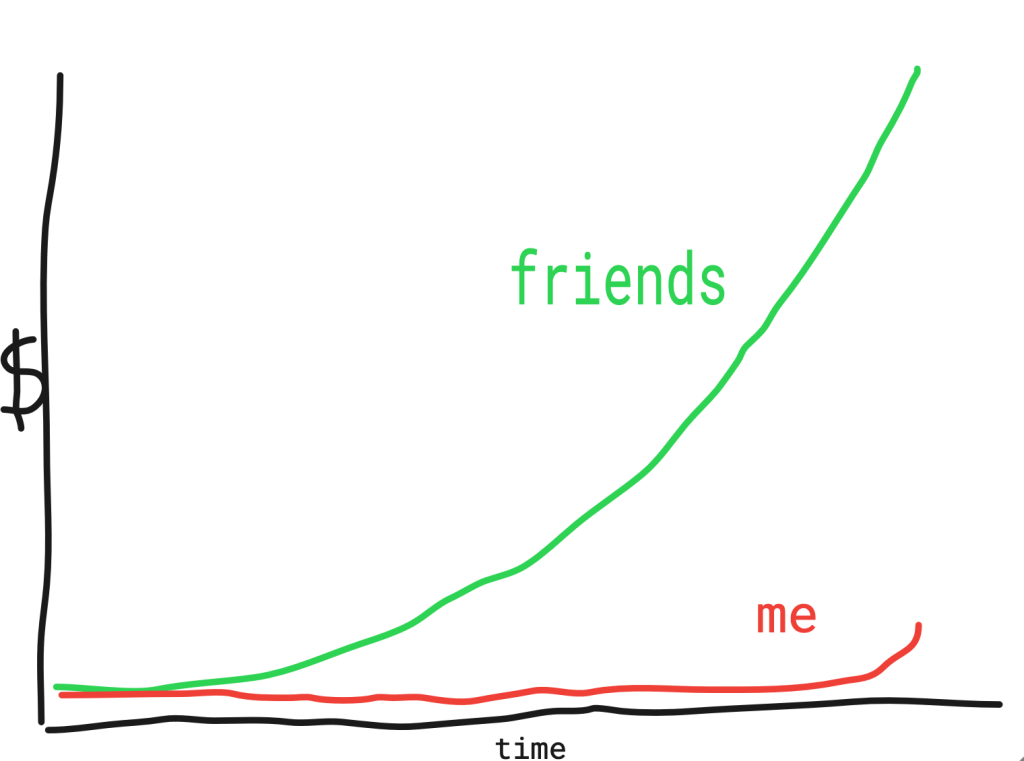
I think it’s important to state that up front, because after eight years of post-medical school training (four residency, two toxicology fellowship) and twelve years of delayed income growth, I’m finally a grown-up making grown-up doctor money. Here is a chart I made showing how far behind my friends I am!
My emergency department administration is remarkably supportive and helped me launch a toxicology consultation service. So I split my time between working ER shifts and doing tox consults. It’s great, especially insofar as it means I work fewer ER shifts.
Continue readingAcademic Publishing is a Massive Corrupt Scam, Pt 2
Since my last post, I have been hard at work like the good little tox minion I am. I have published numerous case reports and gotten my name on others written by my more skillful and motivated co-fellows. I am very proud of these case reports. They accurately reflect my internal cognitive dissonance at Skillfully Playing the Game while also knowing that The Game Is Total Bullshit.
Continue readingAcademic Publishing is a Massive Corrupt Scam
I would like to first point out, before we even get started: after my last post, I had a minor Zoom-based showdown with the HR department about some professionalism modules I was refusing to complete and I got in pretty big trouble. In case you are interested, I stood my ground like the dumpster-inhabiting dipshit I am and ended up NOT HAVING TO DO THE MODULES. F**K YEAH.
Anyway.
Continue readingCataclysEM
I want you to picture a dumpster. A bad one, full of rotting fast food, like a McDonalds-parking-lot-at-3am dumpster. One that no one bothers to lock or protect from animals because even the racoons will stay away from the fermenting, rancid waste.
Got a mental picture? Now place that dumpster aboard a Viking funeral of a ship, ablaze, sailing toward an enormous waterfall with nothing but jagged rocks below.
Continue readingA Bird in the Hand
I will preface this story with a disclaimer: I am not exaggerating the following.
On one short-handed urgent care shift right before Christmas, wait times to see the doctor (me) stretched to four hours, at which point people started a light riot.
The urgent care where I was working normally has two providers at once: an MD and either a nurse practitioner or a physician assistant. That day, the nurse practitioner called out sick with COVID, leaving me alone.
Continue readingYou Must Comply
Guess who graduated residency… but is still in training!?
So now I’m starting my toxicology fellowship. I’m now at a different large academic center, still on the West Coast, and am six weeks in.
Fellowship is going well, except that I wake up every day consumed with a blinding and violent rage – not toward my training program but toward the university’s HR department.
Continue readingPushing Back On Pushback
I was working on writing this gigantic 4,000-word monstrosity of a post where I tried to align specialty services with the old-school Dungeons and Dragons “Lawful/Chaotic vs Good/Evil” axes for character generation, and it was exactly as complicated as it sounds.
As I worked my way through it, I realized that half of what I wrote was about convincing specialists to come down to the ER and see my patients. At large academic centers where we residents train, we are almost always calling other residents for this task – and therein lies the rub. Like us, they are overworked and underpaid a flat salary to do their jobs. When I call the surgery resident for a consult, for example, I am creating work for them.
Continue readingAn ER Doc’s Primer On The COVID Vaccine
Hello! Once again it has been forever, but I don’t care. I’ve been too busy trying to prevent my head from exploding from, once again, people being stupid.
(I am a tiny bit frustrated with vaccine hesitancy, which I sort of understand, and very frustrated with COVID deniers and other conspiracy theorists, who I think should be first boarded onto a 13-hour Spirit Airlines flight and then forcibly ejected out the emergency exits at 35,000 feet.)
Continue readingThe COVIDpocalypse is Here and I’m Coping By Writing Again
I would like to blame my prolonged absence again on COVID-19. To be fair, it does dominate about 95% of my work life and probably 50% of my personal life, but honestly, I’ve just gotten lazy.
The last time I published here was March 5, where I started with “it seems like we are inevitably headed for a massive, global pandemic.” For once on this blog, I get to say I WAS RIGHT ABOUT SOMETHING IN RESIDENCY! No attending or dad can correct this.
As of this writing, my area’s daily hospitalization rates look like a Space-X rocket launch. We’re out of ICU beds, regular beds, gurney, cots, sleeping bags, and patience. The worst is somehow yet to come. I am coping with this impending doom by playing with my dog and, finally, writing again.
Continue reading